Developmental Surveillance & Screening:
Monitoring to Promote Optimal Development
Including next steps if a concern is present or diagnostic workup is indicated
By: Katherine TeKolste, MD, FAAP, Developmental Pediatrician
Overview
Developmental monitoring is an integral part of well-child care.
About 16-18% of all children have disabilities such as intellectual disability, motor disorders, and speech and language disorders. Only half of children with developmental disabilities are identified prior to school entry. And fewer than one in five are enrolled in early intervention services before the age of three years. Well-child exams in the first years of life are ideal for the detection of problems with a child’s development.
Primary care providers’ attention to the developmental progress of children in their practice is critical to the early detection, diagnosis and treatment that leads to opportunities for the best long-term outcomes and optimal child and family functioning.
Parents want and expect support and information on child development, as demonstrated by the Commonwealth Fund, the Healthy Steps Program, the North Carolina Access Project, and CHILD Profile surveys in Washington State, among others.
Resources:
- American Academy of Pediatrics
-
Centers for Disease Control (CDC)
- Developmental Monitoring and Screening for Health Professionals (latest reference is 2010, however page listed as last reviewed on 2.6.19)
- CDC Free Milestone Tracker
- Tips for Talking with Parents About Developmental Concerns – Handout from CDC’s Learn the Signs Act Early
How to Monitor Development in the Primary Care Practice
Assess Risk Factors
Biologic and environmental factors may place a child at higher risk for poor developmental outcome. Children and families for whom these risk factors are present should be monitored especially closely. A child with an established diagnosis associated with a high likelihood of developmental delay (e.g. Down syndrome or autism) should be referred for early intervention services promptly upon diagnosis.
Monitor Development with Surveillance and Screening
Resource for Implementation
- American Academy of Pediatrics Screening Technical Assistance and Resource Center (STAR Center) Information for Practices
References
- AAP December 2019 clinical report with updated recommendations to promote the optimal development of every child.
· Clinical Report: Promoting Optimal Development: Identifying Infants and Young Children with Developmental Disorders Through Developmental Surveillance and Screening - Strategies for Improving Developmental Screening. Whitaker T, Zubler J, et al. Contemporary Pediatrics. 2019 Jan;36(1):5-9.
- Developmental Delay: When and How to Screen. Vitrikas K, Savard D, Bucaj M. Am Fam Physician. 2017 Jul 1;96(1):36-43.
- Improving Developmental Screening Documentation and Referral Completion. Talmi A, Bunik M et al. Pediatrics. 2014;134(4):e1181-e1188.
- Implementing an Early Childhood Developmental Screening and Surveillance Program in Primary Care Settings: Lessons Learned From a Project in Illinois. Berry AD, Garzon DL, et al. J Pediatr Health Care. Nov/Dec 2014;28(6):516-525.
- Coding Corner: How to navigate changes to developmental testing, neurobehavioral status exam codes. AAP Division of Health Care Finance. AAP News. April 2019;22.
Developmental Surveillance
Developmental surveillance is an informal, yet structured monitoring of developmental status over time. The primary care provider must interpret information in light of environmental, social and medical factors affecting the child. Developmental surveillance relies upon information obtained from multiple sources, including assessment of parental concerns and formal developmental screening. Although they should not be the primary method of assessing development, checklists with red flags in development (e.g. milestones that 75% to 90% of children at a given age have achieved) may be useful, especially at interim visits when formal developmental screening is not utilized.
Developmental Screening
Developmental screening is the brief assessment of developmental status utilizing a standardized instrument. The American Academy of Pediatrics recommends that children be screened for general development using standardized, validated tools at 9, 18, and 24 or 30 months and for autism at 18 and 24 months or whenever a parent or provider has a concern.
Detection of developmental problems will never be perfect, even with the standardized screening instruments listed below. All of these screening tools have good psychometric properties including sensitivity and specificity, validity and reliability. Yet, over-referral (child who is sent for further testing and is found to be developing ‘typically’) and under-referral (child with delays who is not identified as needing further assessment) will occur. Under-referrals are minimized by the overall surveillance process, i.e. monitoring development over time.
It is important to recognize that children who are ‘borderline’ in their skills (sometimes included in the ‘over-referral’ group) are at high risk for poorer developmental outcomes even if they do not qualify for early intervention/special education or therapy assistance. A child demonstrating borderline skills should have their developmental growth monitored more closely with more frequent administration of standardized screening tools.
Early involvement in developmental activities, preschool experiences, and other activities can positively impact the child’s learning and achievement. There are resources – from parent websites and handouts, to Head Start / Early Head Start programs and more – that can assist parents and their children with borderline range skills or other concerns.
Examples
- Zero to Three: Make the Most of Playtime
- CDC Milestone Tracker App – includes tips and activities to support child development at every age in early childhood (Available in English and Spanish).
Identification of developmental delay is improved when explicit developmental screening procedures are used.
- Without use of standardized tools only 30% of children with developmental disabilities are identified. This rises to 70-80% of children identified when standardized tools are used. (Refs. Palfrey et al. J Pediatr. 111:651-655, 1987; Squires et al. JDBP. 17:420-427, 1996.)
- Without use of standardized tools only 20% of children with mental health problems are identified. 80-90% are identified with the use of standardized tools (Refs. Lavigne et al. Pediatr. 91:649-655, 1993.; Eisert & Sturner. JDBP. 12:42-50, 1991).
Screen the overall development of all children with a parent questionnaire (at a subset of ages as part of well-child examinations or at each well-child exam, and whenever concerns are expressed).
Parent-completed developmental screening tools
Parental report measures may be administered by interview format and with an interpreter for families where English language literacy is an issue. Several are available in multiple languages.
-
ASQ®-3 – Ages and Stages Questionnaire ®, Third Edition
- The ASQ-3 assesses developmental progress in children between the ages of one month to 5 ½ years (66 months). The questionnaires utilize a parent-centric approach, are easy to use and highlight a child’s strengths as well as concerns. It can be completed at home, in the waiting room, during a home visit or as part of an interview either in-person or by phone.
- Each 30-item questionnaire covers five key developmental areas: communication, gross motor, fine motor, problem solving, and personal-social, plus open-ended questions for vision, hearing and other concerns.
- 21 questionnaires – 2, 4, 6, 8, 9, 10, 12, 14, 16, 18, 20, 22, 24, 27, 30, 33, 36, 42, 48, 54, and 60 months of age and valid from 1-66 months of age. See information on automated questionnaire selection by child’s age at Brookes ASQ® calculator.
- Available in Arabic, English, French, Spanish and Vietnamese.
-
PEDS – Parent’s Evaluation of Developmental Status
- For children birth to 7 years, 11 months of age.
- Ten short questions to parents to elicit concerns about development, behavior and mental health.
- Available in print in English, Spanish, and Vietnamese. Available for licensing in Albanian, Amharic, Arabic, Armenian, Bengali, Bulgarian, Burmese, Cambodian, Chinese (Traditional and Simplified characters), Danish, Dutch, Dzongkha, Farsi, Filipino Tagalog, French, Galician, German, Greek, Gujarati, Haitian-Creole, Hebrew, Hindi, Hmong, Icelandic, Indonesian, Karen, Korean, Laotian, Malay, Nepali, Polish, Portuguese and Cape Verdean, Punjabi,Quechua, Russian, Serbian (Cyrillic and Latin), Samoan, Somali, Sotho, Swahili, Tagalog,Taiwanese, Tamil, Thai,Turkish, Urdu, Vietnamese, Visayan, Yoruba and Zulu.
-
PEDS-DM – Parents Evaluation of Developmental Status – Developmental Milestones
- Ages birth to 7 years 11 months; 6 to 8 items per age/encounter; Each item taps a different developmental domain (fine motor, gross motor, expressive language, receptive language, self-help, social-emotional, and for older children – reading and math)
- Available in English and Spanish. Licensed translations available in Arabic, Chinese, French Canadian, Japanese, Korean, Punjabi, Swahili, Taiwanese, Tamil and Thai.
-
SWYC – Survey of Well-Being of Young Children
- Free screening instrument for children under 5 years of age.
- Every SWYC form includes sections on developmental milestones, behavioral/emotional development, and family risk factors. At certain ages, a section for Autism-specific screening is also included.
- Translated into Spanish, Khmer, Burmese, Nepali, Portuguese, Haitian-Creole and Arabic.
Accuracy of Parental Report Measures
- Parents are often INACCURATE on recall of milestones (e.g. When did your child first wave bye-bye?).
- Parents are ACCURATE on reporting of current skills.
- Parental concerns are ACCURATE indicators for:
- Speech and language delays
- Fine motor delays
- General delay
- Parental concerns are LESS ACCURATE indicators in the areas of:
- Self-help skills
- Behavior
Reference: Glascoe FP. Parents’ concerns about children’s development: prescreening technique or screening test? Pediatrics. 1997. 99(4):522-528.
Flow Sheet for Developmental Screening
[Courtesy of Nickel RE and Squires J. In The Physician’s Guide to Caring for Children with Disabilities and Chronic Conditions. Eds. Nickel RE, Desch LW. PH Brookes Publishing Co. (2000): p. 22.]
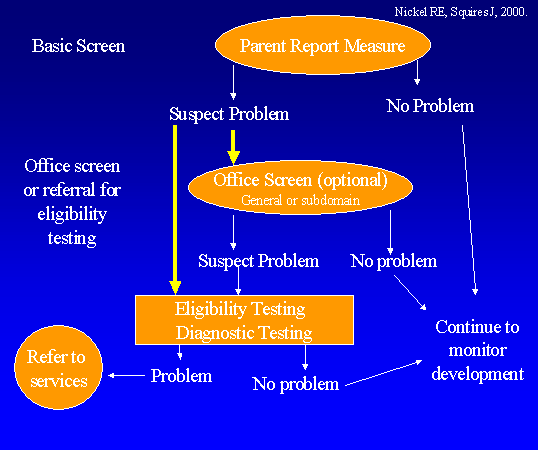
What To Do After The Screening – Next Steps
1. Talk with parents about results
2. Parents as Partners – Monitoring and Referral
3. If unsure, REFER!
Talk with Parents About Results
- Emphasize child’s current skills
- Emphasize family skills & resources
- Discuss current screening results
Typical Development / No Concerns
Continue routine monitoring.
Minor Concerns
No pathology present but child demonstrates immaturity in skill level or quality.
- Children’s developmental pattern may show bursts and plateaus
-
Assess risk factors
- Development is influenced by health and environmental factors. For example, since implementing the back-to-sleep recommendations, infants may show immaturity of head control in prone position.
- Some risk factors put a child at higher risk, e.g. very-low-birth-weight infant or infant with microcephaly.
- Determine whether immediate referral for assessment is indicated or whether the child should continue to be monitored with another developmental screening in a month or two. If unsure, refer for assessment.
- Consider need for hearing or vision assessment.
- Schedule recheck appointment
More than Minor Concerns
- Concerns identified on screening are NOT confirmation of a problem but only an indicator of the need to look further.
- Indicate to the parents / caregivers the need for further assessment (developmental assessment, hearing, vision, other) and make arrangements.
- Hints on discussion concerning screening results:
See ‘Sharing Sensitive News’ including resources at bottom of section.
Give Parents Activities, Monitoring Tools and Resources
Parents as Partners – Monitoring and Referrals
- Give parents activities to enhance development, tools to continue to monitor developmental progress, and resources for child development information.
Activities and Information Resources
- Zerotothree.org
- Child Profile Health and Safety Information for Parents and Caregivers
-
Parenting Counts
- Developmental Timeline and activities
- ABC’s of Child Development
- PBS Parents
Tools to Monitor Development
- Help Me Grow Washington (English or Spanish)
- Free developmental screening for all kids under 5 (no waiting lists or income requirements)
- Activities and games that support healthy growth and learning
Community resources like parenting classes, medical clinics, and food banks - Referrals for further evaluation and early intervention services
- CDC Milestone Tracker App – in English and Spanish
- Easter Seals Make the First Five Count –
- Ages and Stages Questionnaire Screening in English
2. Consider referral to programs such as infant-toddler play groups, preschool programs, Early Head Start and Head Start programs, and parenting programs.
ParentHelp123.org Resource Finder or call the Family Health Hotline 1-800-322-2588
3. Consider developmental stimulation activities and programs
- “Reach Out and Read” – find Washington State Programs
- Storytimes – library, local bookstores, other
- Information about books and early literacy for young children
Community partners for further screening and linking to services.
- 0-3 years old – Family Resources Coordinators in the Support for Infants and Toddlers (ESIT) Program
- 0-18 years – Children with Special Needs Coordinator in the local Public Health Department/District (Usually a public health nurse)
- 3-21 years – the local School District Special Education program or Child Find can help.
You can find also local contact information through the WithinReach Family Health Hotline 1-800-322-2588 or their website.
- Further evaluation to confirm or refute presence of delays
- If delay is confirmed:
-
- Connect with interventions
- Work up for developmental delay/ intellectual disability- Establish etiology, if possible
- Assist parents – Information and support
- Coordinate care
- Refer, as needed, to medical specialists
-
If Unsure, REFER
Confirm/rule out the presence of delays or atypical development
- Refer for further assessment
- In the state of Washington, either of the following people can link you to resources for further developmental assessment in your community.
-
County Resources
See sections listing:
– CSHCN Coordinators (serving children 0-18 years of age)
– Family Resource Coordinators (serving children 0-3 years of age).
Provider Assessment
- Families can the Washington State Family Health Hotline at 1-800 322-2588 or 1-800-833-6388 (tty relay) and be linked to resources for further assessment.
- Give parents information about the assessment process
If Child is Not Delayed/Not Eligible for Services :
- Recommend activities and resources to enhance development (see Parents as Partners section immediately above this section)
- Continue to monitor the child’s development closely.
If Delay is Confirmed:
1. Connect with Interventions and Supports
- 0-3 Family Resources Coordinators (FRCs), Children with Special Health Care Needs (CSHCN) Coordinators from the local health department, Neurodevelopmental Centers and other county resources
- Connect the family with the toll-free state maternal and child health hotline WithinReach 1-800 322-2588 or 1-800-833-6388 (tty relay).
- WithinReach can connect the family with support for parents, fathers, siblings and others.
- Family Resources Coordinators- FRCs help families access all Part C of the Individual with Disabilities Education Act (IDEA) services the child and family need as identified in the Individualized Family Service Plan (IFSP) and assist in coordinating early intervention services with other services needed by the child, such as medical care or durable medical equipment.
- Neurodevelopmental Centers
The Neurodevelopmental Centers of Washington (PDF) are a group of 19 community non-profit and hospital-based agencies who provide therapy and related services to young children with neuromuscular or developmental disorders. The centers are located across the state, each one meeting needs specific to its community. - Public Health Children with Special Health Care Needs Coordinators
Washington State Department of Health has CSHCN Coordinators located in each of the 34 health districts. The coordinators are generally public health nurses. They provide services to children birth to 18 years of age who reside in Washington State and who have or are at risk of having a serious physical, developmental, behavioral or emotional condition and who require health and related services beyond that generally required.
-
- Helps families access needed services for their child such as medical care and treatments.
- Refers families to health insurance programs and information.
- Helps families find support through parent organizations.
- Assists with concerns related to feeding, nutrition, growth and development.
2. Establish etiology, if possible
-
Why?
- Estimation of recurrence risk,
- Prognosis,
- Medical follow-up for known complications,
- Specific therapeutic interventions – available in rare cases
-
Resources:
- Information for families about pediatric subspecialties
- Neurodevelopmental centers in Washington
- List of Hospitals statewide
-
Newborn Screening – Condition-specific Action Steps and Treatment Algorithms
- An ACTion (ACT) sheet describes the short term actions a health professional should follow in communicating with the family and determining the appropriate steps in the follow-up of the infant that has screened positive.
- An algorithm that presents an overview of the basic steps involved in determining the final diagnosis in the infant. The algorithms were developed by a work group that included experts in the various specialties and conditions involved in newborn screening for endocrine, hematological, genetic and metabolic diseases.
- All materials were approved by the Board of Directors of the American College of Medical Genetics (ACMG). The materials will be maintained by ACMG over time and additional materials added as new conditions are introduced into newborn screening programs
- Dysmorphic features list –
- Dymorphology assessment of the newborn
-
Additional Etiologic Work Up Information:
- Laboratory Testing: Array-based Comparative Genomic Hybridization(CGH)- general information for physicians
- Genetic and Metabolic Testing in Children with Global Developmental Delay: AAN report (AAP Endorsed) March 2012.
-
References for Evaluation of Developmental Delay:
- Clinical Report: Identification, Evaluation, and Management of Children With Autism Spectrum Disorder – from the Council on Children with Disabilities and Section on Developmental and Behavioral Pediatrics, published in the January 2020 issue of Pediatrics.
· Clinical Report: Identification, Evaluation, and Management of Children With Autism Spectrum Disorder
· Executive Summary - Clinical Genetic Evaluation of the Child with Mental Retardation or Developmental Delays. Moeschler JB et al. (AAP Committee on Genetics) Pediatrics. 117:2304-2316, June 2006.
- A Rational Approach to the Medical Evaluation of a Child with Developmental Delay. Roberts G, Palfrey J, Bridgemohan C. Contemporary Pediatrics.21(3):76-99, March 2004.
- Developmental Delay in Children Younger than 6 Years. Davis BE, Bennett FC. In Pediatric Decision Making, 4th Edition. Ed. Berman S., Mosby, Philadelphia, 2003.
- Developmental Delay: When to suspect and how to investigate for an inborn error of metabolism. Cleary MA, Green A. Arch Dis Child. 90:1128-1132, 2005.
- Diagnostic Evaluation of Developmental Delay/Mental Retardation. Battaglia A, Carey JC. Am J Med Genet. 117C:3-14, 2003. (See the “algorithm for ‘rational evaluation’ of a patient with MR/DD” in Figure 1).
- Developmental Delay and Mental Retardation. Nickel RE. In The Physician’s Guide to Caring for Children with Disabilities and Chronic Conditions. Nickel RE, Desch LW. Eds. Paul H. Brookes Publishing Co., 2000.
- Identification and Evaluation of Mental Retardation. Daily DK, Ardinger HH, Holmes GE. American Fam Physician. 61(4):1059f. 2000.
- Clinical Report: Identification, Evaluation, and Management of Children With Autism Spectrum Disorder – from the Council on Children with Disabilities and Section on Developmental and Behavioral Pediatrics, published in the January 2020 issue of Pediatrics.
3. Assist parents
Provide information and support for family and child with developmental delay.
- Key Contacts such as FRCs and CSHCN Coordinators
- Family Support
- Washington State Resources by County
4. Coordinate care
Link children with special health care needs and their families to services and resources in a coordinated effort to maximize the potential of the children and provide them with optimal health care (AAP, Committee on Children With Disabilities, 1999).
Early Intervention WORKS!
- Windows for learning begin at birth.
- There are greater developmental gains with less chance of secondary problems when early intervention begins soon after diagnosis.
-
- Early intervention reduces the need for special education and other services later in life
- In Washington State over 8,900 children received birth-to-three early intervention services from October 1, 2007– September 30, 2008. In the same period, 4,097 children transitioned out of early intervention services. Of these 4,097 children, 1,094 or 27.0% no longer needed special education services.
- Early intervention reduces the need for special education and other services later in life
- Early intervention reduces additional stressors on families.
- Early intervention is cost-effective.
For more information on early intervention programs see:
- CLINICAL REPORT: Early Intervention, IDEA Part C Services, and the Medical Home: Collaboration for Best Practice and Best Outcomes. Richard C. Adams, MD, Carl Tapia, MD, and THE COUNCIL ON CHILDREN WITH DISABILITIES. Pediatrics (2013) www.pediatrics.org/cgi/doi/10.1542/peds.2013-2305
Listen to Concerns from Parents and Others Who Know the Child
When a parent expresses concern about a child’s development, there is a good chance there is something that needs attention.
Parental concerns are particularly likely to be accurate in the areas of speech and language skills, cognitive performance, and fine motor skills.
When parents gather at ‘Conversations with Families’ [a discussion and networking forum for families participating in early intervention services (Early Support for Infants and Toddlers) in Washington state], a theme repeated throughout the state is the parents’ perception of having been worried about their child’s development but not feeling heard by their health care provider when those concerns were expressed. Similar concerns have been noted by Head Start providers who indicate having screened a child’s development and suggested parents follow up with a medical provider only to have the concerns minimized or dismissed.
It is also important to recognize that 20-25% of parents do not raise concerns when delays are present.
More information: Glascoe FP. Parents concerns about children’s development: prescreening technique or screening test? Pediatrics. 1997. 99(4):522-528.



